The hysterosalpingogram (HSG) test is a test to determine if your fallopian tubes are blocked. If they are, sperm won’t be able to reach the egg and if sperm somehow made it through, the fertilized egg wouldn’t be able to get to the uterus.
I completely worked myself up for this ordeal by talking to people that had this test done, and of course, looking it up online and on social media. I learned that their stories were contradictory – from not feeling anything at all to the most excruciating pain that made them blackout. I intended to get reassurance to feel more prepared, but that backfired.
Everyone’s experience is so different, so if you’re going to do this test too, here’s some sound advice: Don’t talk to anyone except your doctor about it and stop reading this post. 😅
The nurse from my RE’s office instructed me to take Aleve 30 minutes to 1 hour prior. I took 2 Aleve pills 45 minutes before. I think this is important to mention because I know two women that did not take a pain reliever beforehand and they had horror stories.
My HSG test was done in the radiology department with three doctors – my Reproductive Endocrinologist, a Radiologist, and another doctor just for fun. Haha, I don’t know actually why the other doctor was there. Plus a nurse and a radiology student.
At first, the procedure was similar to a normal papsmear. I laid on my back on the exam table with my knees bent and feet up on the edge of the table because this table didn’t have stirrups. My RE inserted a speculum into my vagina and cleaned my cervix. That’s where the similarity and familiarity ended.
It was good to have my RE, instead of a Radiologist do the test because she is very experienced and knew that my cervix is tilted. BUT she didn’t remember which way it was tilted so when she put in the catheter it took her two attempts. She said she’s usually a one try kind of girl and for me to remember the positioning 2:00. It felt like a sharp pain. See my face below for reference.
She removed the speculum and the nurse and student dragged the sheet under me so I slid up on the table and was positioned under the fluoroscopy camera. My RE waited for the Radiologist to be ready before she blew up the tiny ballon at the end of the catheter to the size of a pea. That sounds tiny, but it felt huge inside of me. Then she filled my uterine cavity, fallopian tubes and peritoneal cavity with dye from the catheter. When the dye was filling my fallopian tubes it felt like EXTREMELY bad cramps, but only for one minute. Once it was over it felt like normal period cramping. When the dye was going through my fallopian tubes, the Radiologist was taking the fluoroscopic images.
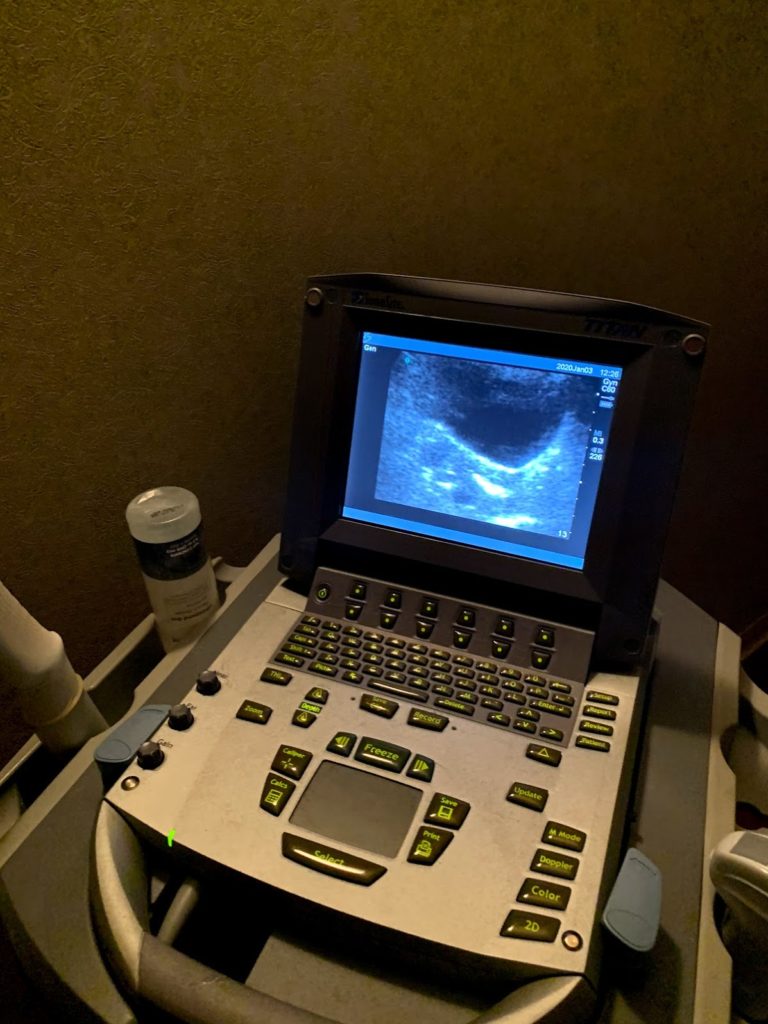
It was also good to have my RE do it because she saw the results instantaneously. She said my left fallopian tube was totally clear because the dye spilled out quickly. She wasn’t sure about my right tube so I had to roll all the way over and back onto my back to move the dye around and get more images taken, then she saw that my right tube was open too.
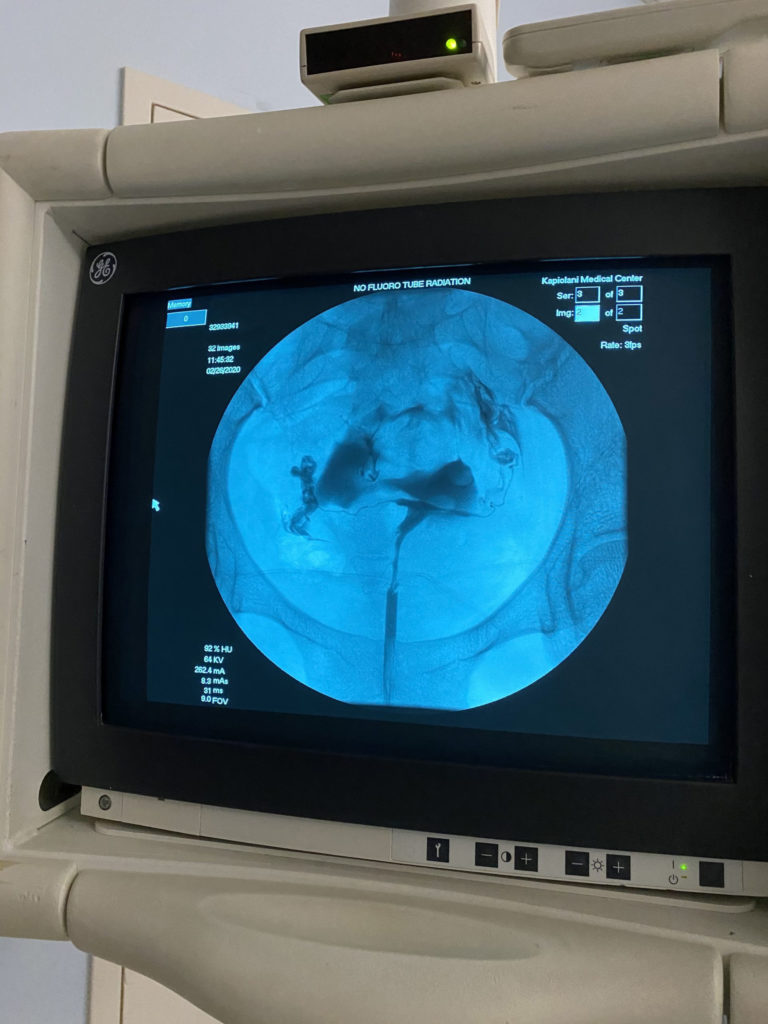
Side note: I was annoyed that no one told me there is a possibility of spotting because I would’ve brought my period panties with me. Sustainability! I had to use one of their huge, thick pads that probably was equivalent to more than 3 plastic bags.
I went to my RE’s office afterwards to have an ultrasound done to see how the Letrozole I took last week has been working. I took this fertility drug again to prepare for another IUI if my tubes are open. The ultrasound confirmed that the dye leaked out of my tubes, showed that my follicles were growing and on their way to be ready for ovulation, and that the egg would be coming from the left fallopian tube this cycle. This is perfect since my left tube was very clear.
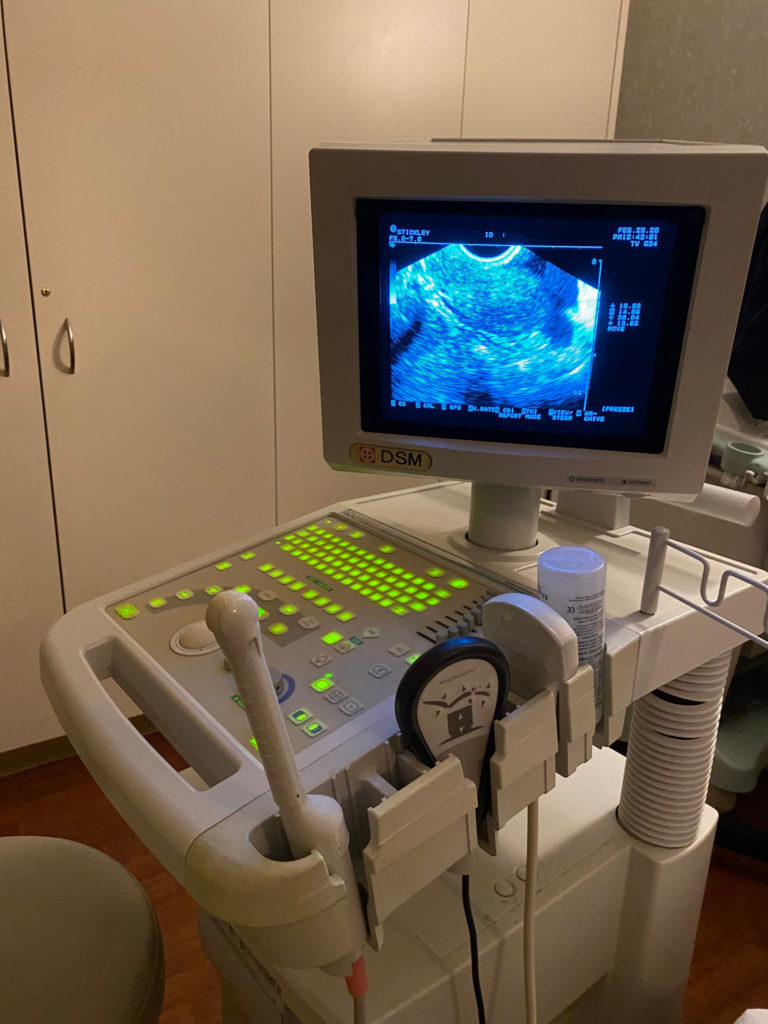
About an hour later, I was lightheaded and then had a bad headache. I slept on and off for the rest of the day. I’m writing this the day after. I’m cool now.